Eczema is a complex and pervasive skin disorder affecting countless individuals around the globe. Manifesting as reddened, itchy patches, it often diminishes an individual’s daily life quality. Central to managing this persistent itch is the judicious application of eczema creams. However, navigating the world of these treatments is not without its pitfalls. Misuse of certain creams, particularly steroids, can plunge a patient into the agonizing realm of Topical Steroid Withdrawal (TSW). This article seeks to demystify the art and science of eczema cream application, providing insights into the avoidance of TSW’s debilitating effects.
Page Contents
Understanding Eczema

Eczema, an umbrella term for a cluster of skin conditions, presents itself in several forms, the most common being atopic dermatitis and contact dermatitis. These conditions manifest as inflamed, itchy, and often scaly patches of skin. Triggers for eczema flare-ups can be diverse, ranging from environmental allergens, such as pollen and dust mites, to stress and hormonal fluctuations. Though genetic predisposition plays a significant role, external factors can exacerbate symptoms. Management demands a comprehensive understanding of the condition, and central to this understanding is the role of moisture, barrier repair, and inflammation control in treatment.
Types of Eczema Creams
The market offers a diverse range of eczema creams tailored to address various facets of the condition. Broadly, these can be categorized into corticosteroid creams, moisturizers, and barrier creams. Corticosteroids act primarily to reduce inflammation, providing rapid relief from acute flare-ups. Moisturizers serve to hydrate the skin, restoring its natural barrier function and reducing susceptibility to irritants. Barrier creams create a protective layer on the skin’s surface, shielding it from potential triggers. Selecting the appropriate cream hinges on a clear understanding of its purpose and the specific needs of one’s skin condition.
Consulting a Dermatologist
Navigating eczema’s complex landscape can be daunting, necessitating expert guidance. A dermatologist, specialized in skin disorders, can be an invaluable ally. Beyond diagnosing the specific type of eczema, they can recommend tailored treatments, optimizing outcomes. The importance of personalized advice cannot be overstated. What works for one individual may not work for another. Moreover, with a plethora of products available, identifying the most effective and safest option requires professional expertise. In situations where over-the-counter solutions falter, a dermatologist may prescribe more potent treatments or adjust existing regimens.
Selecting the Right Eczema Cream

Selecting an eczema cream is more intricate than simply grabbing a product off the shelf. Firstly, understanding one’s skin type—be it oily, dry, or combination—is crucial. Next, reading product labels is essential. They provide insights into active ingredients, potential allergens, and intended usage. Some creams might contain fragrances or preservatives, which could exacerbate eczema in sensitive individuals. Moreover, consider the severity of your eczema and any known triggers. With these factors in mind, selecting a cream that aligns with your skin’s needs becomes a more informed process.
Proper Application Techniques
The efficacy of an eczema cream isn’t solely about the product itself—it’s also about its application. Begin with clean hands and pat-dry the affected area. When applying, use gentle, upward strokes, ensuring even distribution. It’s crucial to apply creams on slightly damp skin, often after a shower, to lock in moisture. Avoid vigorous rubbing, which can irritate the skin further. For areas with thicker skin, like elbows, a more generous amount might be required. By adhering to these techniques, the absorption and effectiveness of the cream can be maximized, providing optimal relief.
Frequency of Application
When it comes to applying eczema creams, there isn’t a one-size-fits-all answer. The frequency is influenced by various factors including the specific cream composition, the aggressiveness of the eczema, and the unique characteristics of an individual’s skin. For example, moisturizers, which provide hydration, often demand more frequent application, especially when the atmosphere is dry such as in colder months or arid regions. In contrast, potent corticosteroid creams are typically prescribed for shorter cycles to prevent potential complications. It’s essential to monitor skin reactions closely. Any signs like increased redness or irritation might necessitate a reconsideration of how often you apply the product or a prompt consultation with a skin expert.
Avoiding TSW
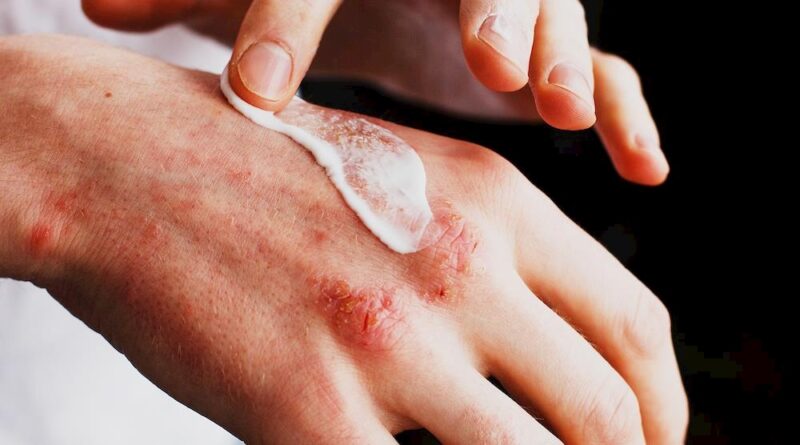
Topical Steroid Withdrawal (TSW) is an adverse reaction that some face after extended, unsupervised use of corticosteroid creams. It’s marked by symptoms like severe redness, the appearance of small blisters or pustules, and an almost unbearable itchiness. The path to TSW can be a slippery slope, which is why it’s paramount to apply steroid creams as directed by a dermatologist. Sticking to the advised duration of use and resisting the temptation to use a more potent cream than suggested is essential. If there’s a suspicion of TSW onset, it’s imperative to get medical attention without delay. It’s worth noting that stopping corticosteroids suddenly may not always be beneficial; sometimes, a phased reduction under the watchful eye of a dermatologist is the best approach.
Alternatives to Steroid Creams
While steroids are undeniably potent in curbing eczema symptoms, they aren’t the only available treatment. Many seek alternative non-steroidal options, and among these, calcineurin inhibitors stand out, offering relief without the steroid-associated risks. In the realm of natural treatments, remedies like calming oatmeal baths or the application of coconut oil have received considerable attention and praise from those who prefer a more organic approach. Yet, while these natural treatments can be effective and gentle, it’s of utmost importance to remember that ‘natural’ doesn’t mean universally safe. An individual’s skin might react differently, so caution, and if possible, a dermatologist’s input, is always recommended when exploring alternative treatments.
Managing Eczema Holistically
Beyond creams, eczema management demands a holistic approach. Diet plays a pivotal role—certain foods can either trigger or alleviate symptoms. Similarly, stress, known to be an eczema aggravator, must be managed effectively. Techniques like meditation or yoga can be instrumental. Additionally, wearing breathable fabrics, maintaining a regular sleep pattern, and ensuring a clean living environment can cumulatively mitigate flare-ups. Thus, a multifaceted approach often yields the best outcomes.
Monitoring and Adjusting

Consistent monitoring of eczema symptoms and treatment efficacy is vital. Not all treatments work uniformly for everyone. If a particular cream or regimen doesn’t yield expected results or exacerbates symptoms, reevaluation is necessary. Documenting daily skin responses can provide valuable insights. If persistent irritation or unexpected reactions occur, seek professional counsel. Adjusting treatment plans based on evolving skin needs can ensure sustained relief.
Conclusion
Eczema, though challenging, is manageable with the right approach. Safely applying creams, being aware of potential pitfalls like TSW, and adhering to holistic management strategies can significantly enhance life quality. Always prioritize skin health, seek expert advice, and remember: informed, consistent care is the cornerstone of effective eczema management.